
Arnaud Petit
Arnaud Petit, doctor and leader of the “Mannequin patients for future doctors” project
Here the watchwords are “never the first time on the patient” for learning invasive procedures
Tell us about your work and your project.
I'm a university professor of pediatrics at Sorbonne University and a hospital practitioner in the pediatric hematology and oncology department at Armand Trousseau Hospital. Since 2012, I've been tasked with developing simulation in pediatrics for the second cycle of medical studies. To this end, the Faculty of Health Sciences equipped us with our first high-fidelity pediatric mannequin. Then, in 2017, we obtained our first grant from the Ile de France region’s Health Agency (Agence régionale de santé Île-de-France), which enabled us to create the P2ULSE (Plateforme Pluridisciplinaire hospitalo-Universitaire de e-Learning et de Simulation dans l'Est parisien) healthcare simulation platform thanks to the provision of unused operating theatres. The "Drôles de patients pour futurs médecins" ("Mannequin Patients for Future Doctors") grant, followed by other subsidies, notably from the Île-de-France region and other associations, enabled us to add to our equipment and take a concrete step towards the teaching of the future. Simulation-based learning on mannequins is now an essential part of health sciences.
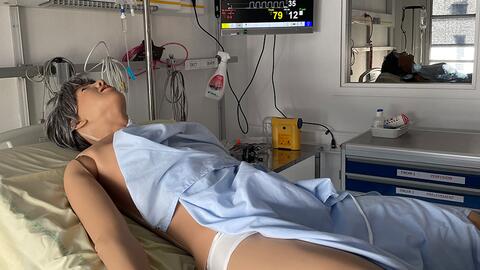
Mannequin utilisé sur la plateforme P2ULSE pour les séances de simulation des étudiants en santé
How important is the use of mannequins in learning to care for patients, especially children?
The “Mannequin Patients for Future Doctors” project has enabled us to expand our training offering and ensure that every medical student practices pediatric lumbar punctures on newborn mannequins funded by donors. Since 2018, all 5th-year medical students have been trained through procedural simulation on these mannequins. Students follow an online theoretical training module, followed by learning the gesture, and then a final assessment to ensure that the gesture and knowledge have been acquired. Providing them with this equipment has enabled us to set up a training program that combines theory and practice to develop their skills.
More generally, simulation enables future professionals to prepare for the rare situations they may face one day. They must be able to recognize and react to such situations. Enabling learners to prepare themselves to act in simulated care situations is part of a logic of care safety. Through structured debriefing, they are encouraged to reflect collectively on care processes and their own emotional mechanisms (stress and emotion management). The realism of the mannequins helps to immerse them in the simulated situation.
We are also working to pass on the values and practices of interprofessional cooperation, for example by involving both medical and nursing students in the same simulation sessions. This enables them to work on group cohesion, and the way in which critical information is transmitted safely for the benefit of the patient.
Finally, the watchwords here are "never the first time on the patient" when it comes to learning invasive procedures. Simulation prepares us better for patient care. It complements "bedside" training.

Salle de formation avec des mannequins de nouveaux nés
What message do you have for all our donors who have committed to the project?
I'd like to thank them. Their generosity has helped to transform our teaching by integrating simulation. They will have contributed to the training of tomorrow's student nurses and doctors, whom we will all need at some point in our lives.
What impact has the project had on students at Sorbonne University's Faculty of Health Sciences?
The students are very satisfied and their feedback is excellent. Since the start of our simulation activities, we've been using a systematic questionnaire to get feedback from students. This feedback has enabled us to improve certain simulation sessions.
The sessions dedicated to pediatrics are very much appreciated. They reassure students who are not used to dealing with children. Indeed, the medical curriculum is very much geared towards adult pathologies. These sessions take place at the same time as their pediatric internship, giving them a better immersion in the "pediatric" world.
In 2022, P2ULSE organized 338 simulation sessions, benefiting some 1,800 students.

Vue de la régie d'où sont commandés les mannequins utilisés pendant les séances de simulation
Do you have other projects planned?
Our ambition is to maintain our offer of simulation-based teaching during health studies. P2ULSE also aims to maintain and develop skills throughout the professional career of hospital caregivers. These continuing education programs are in line with our missions. They play a key role in the transformation of our healthcare services to the benefit of patients.
The future of simulation also means the development of electronic simulation, and both augmented and virtual reality. Student learning is facilitated when teaching approaches are diversified. Lecture courses are still well suited to the transmission of certain types of knowledge, while procedural, electronic and hybrid simulation techniques open up new learning objectives, focusing more on know-how and interpersonal skills. These new forms of simulation-based learning will not replace bedside training, but they are complementary. Hospital internships are a further stage in the peer learning process, prior to the assumption of responsibility in a few years' time.
Simulation is not a magic tool. It prepares, it reassures. It will help us to be as responsive as possible, as ready as possible, to deal with the complexities of the patients we will be faced with. Medicine is a demanding, exciting, day-to-day apprenticeship that is enriched throughout a career.
You can support our healthcare projects
Advances in healthcare engineering and the development of medical humanities are leading to new medical approaches, both in terms of the procedures used and in terms of understanding the patient and his or her freedom. Contribute to these advances by supporting the Sorbonne University Foundation.
Harry Sokol
Gastro-entérologue et spécialiste du microbiote intestinal
Nous avons été parmi les premiers à mettre en évidence scientifiquement les altérations du microbiote chez les patients atteints de Mici.

